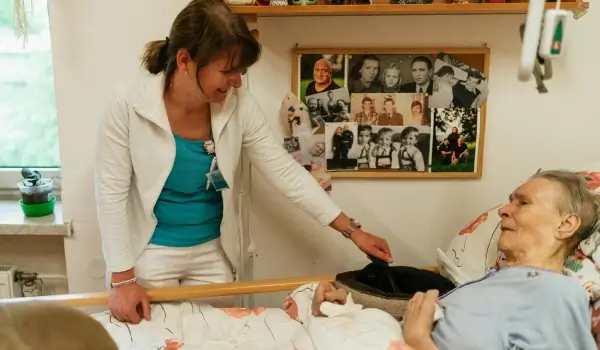
When people hear the term palliative care, many mistakenly equate it with end of life care. This misconception prevents countless patients and families from accessing a resource that could dramatically improve their quality of life right now. Palliative care is specialized medical care focused on relieving the symptoms and stress of serious illness, regardless of the diagnosis or stage of disease. Beyond its primary goal of comfort, one of its most significant and measurable benefits is a substantial reduction in costly, disruptive hospitalizations.
Proactive Symptom Management at Home
The most direct way palliative care reduces hospital admissions is through aggressive, proactive symptom management. Patients with serious illnesses like advanced heart failure, chronic obstructive pulmonary disease, or cancer often experience distressing symptoms such as pain, severe shortness of breath, nausea, and anxiety. Without a dedicated team managing these issues at home, these symptoms escalate until they become emergencies, prompting a frantic trip to the emergency room.
A palliative care team works continuously with the patient and family to stay ahead of these symptoms. They adjust medications, teach nonpharmacologic coping strategies, and provide clear instructions on what to do when symptoms flare. This 24/7 access to expert guidance gives patients an alternative to the emergency department. They learn to manage a breathing crisis at home with the right medication adjustment or breathing technique. This proactive approach transforms a terrifying, symptom driven event into a manageable, home based intervention.
Care Coordination and Communication
Fragmented care is a leading cause of preventable hospitalizations. Patients with complex conditions often see multiple specialists who do not communicate effectively with one another. This lack of coordination leads to conflicting instructions, duplicate tests, medication errors, and delayed treatment of emerging problems. By the time these issues compound, hospitalization becomes inevitable.
Palliative care teams function as expert navigators and communication hubs. They maintain contact with the primary care physician, cardiologist, oncologist, and home health agencies. They ensure everyone works from the same care plan and that the patient’s goals remain central to all decisions. This coordination extends to advanced care planning. When patients have honest conversations about their wishes and complete advance directives, they are far less likely to end up in an intensive care unit receiving unwanted, aggressive interventions. They receive care aligned with their values, which often means avoiding hospital admissions that do not align with their goals.
Family Caregiver Support and Confidence
Hospital readmissions frequently result from exhausted, unprepared family caregivers reaching a breaking point. Caring for a seriously ill loved one at home is physically demanding and emotionally overwhelming. Without adequate training and support, caregivers miss early warning signs of decline, struggle to administer complex medication regimens, and eventually succumb to burnout. This collapse of the home support system forces a hospitalization.
Palliative care addresses this directly by treating the family as part the unit of care. Teams educate caregivers on what to expect, teach them practical skills, and provide emotional support. They validate the difficulty of the role and offer respite resources. A confident, supported caregiver is far more capable of managing a difficult night or a concerning symptom without calling an ambulance. By strengthening the entire home ecosystem, palliative care keeps patients safely where they want to be, surrounded by the people they love, and out of the hospital bed they fear. This is the quiet, powerful work of palliative care happening every day in homes across the country.