Understanding the Goals of Palliative Care
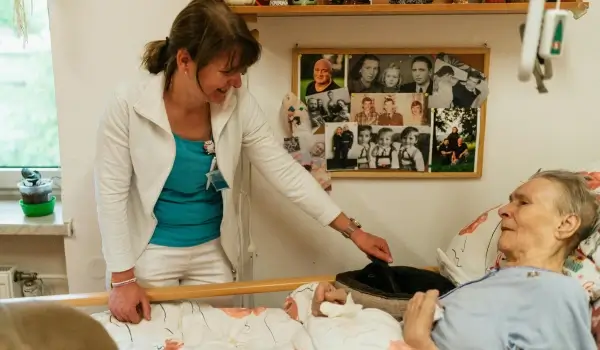
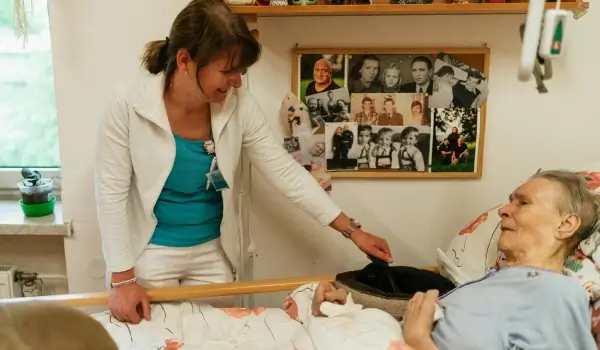
Palliative care is one of the most misunderstood areas of medicine. Many people assume it is only for those who are actively dying, or that choosing it means giving up on treatment. In reality, palliative care is about something much broader: improving the quality of life for anyone living with a serious illness, at any stage of that illness, alongside any other treatment they may be receiving.
Relieving Pain and Managing Symptoms
The most immediate goal of palliative care is to reduce suffering. This means addressing physical symptoms like pain, nausea, fatigue, shortness of breath, and sleep disturbances that often accompany serious illness. A palliative care team works to find the right combination of treatments to keep the patient as comfortable as possible. When symptoms are well managed, people have more energy and mental clarity to engage with their lives, their loved ones, and other aspects of their care.
Supporting Emotional and Psychological Wellbeing
A serious diagnosis affects far more than the body. Anxiety, depression, grief, and fear are common experiences for patients and their families. Palliative care teams typically include social workers, counselors, and chaplains who help patients process what they are going through and find sources of meaning and strength. If you are looking for that kind of compassionate, whole-person support, visit https://signaturehch.com/bellingham/ to learn how Signature Home Care in Bellingham approaches palliative care. Emotional support is not a secondary concern in palliative care; it is built into the foundation of the approach.
Helping Patients and Families Make Informed Decisions
Serious illness often brings complex medical decisions. Palliative care specialists are skilled at facilitating honest, compassionate conversations about prognosis, treatment options, and what the patient values most. These conversations help align medical care with the patient’s personal goals, whether that means pursuing aggressive treatment, focusing on comfort, or finding a balance between the two. Families benefit from this clarity as well, especially when decisions need to be made on behalf of a loved one.
Providing Care Across the Illness Journey
Unlike hospice, which is specific to end of life, palliative care can begin at diagnosis and continue through treatment, recovery, or disease progression. It adapts as the patient’s needs change. This continuity ensures that quality of life remains a priority at every stage, not just when curative options have been exhausted.
Palliative care does not signal the end of hope. It signals a commitment to living as fully as possible, regardless of the medical circumstances.…